Stem Cells
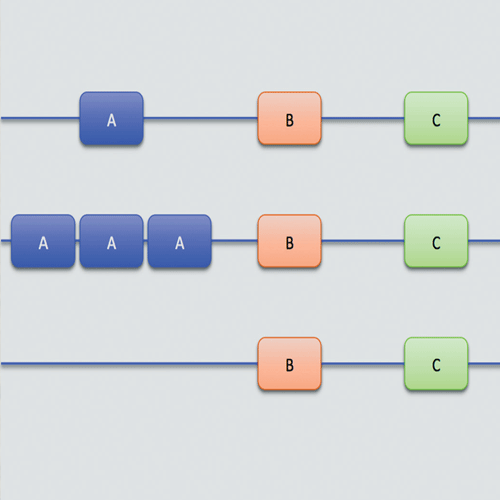
 Stem cells can be thought of as master cells, the raw materials from which a complete individual is crafted. The power of a stem cell lies in its pluripotency – the ability to divide and develop (differentiate) into any one of the 220 various types of cells found in the body. As cells differentiate, they lose this ability: a liver cell, for example, can only renew itself to form more liver cells – it cannot become a lung or brain cell.
Stem cells can be thought of as master cells, the raw materials from which a complete individual is crafted. The power of a stem cell lies in its pluripotency – the ability to divide and develop (differentiate) into any one of the 220 various types of cells found in the body. As cells differentiate, they lose this ability: a liver cell, for example, can only renew itself to form more liver cells – it cannot become a lung or brain cell.
Because of this pluripotency, stem cells have great medical potential. They could be used to recreate insulin-producing cells in the pancreas to treat Type I diabetes, to repopulate neurons destroyed due to Parkinson disease or to replace cells lost in spinal cord injuries. In the laboratory, stem cells have been used to successfully treat animals affected with paralysis, muscular dystrophy, Parkinson disease and sickle cell anemia.
Multiple types of stem cells have been identified or developed. Embryonic stem cells (ES cells) were the first category discovered. These cells are fully pluripotent, but only found in young embryos (the stage of human development from conception to eight weeks gestation). Because the process to collect ES cells destroys the embryo, some groups are opposed to their use.
In the tissues of many developed organs, scientists have identified so-called adult stem cells that retain a portion of the ability to differentiate into other cell types. The primary role of adult stem cells is to maintain and repair the tissue in which it is found. For example, bone marrow contains adult stem cells, which can give rise to all the types of blood cells. This is why a bone marrow transplant can repopulate the blood and immune cells in a patient. It appears that adult stem cells may not have the full range of pluripotency found in ES cells, although researchers are exploring techniques to use adult stem cells for certain forms of therapy.
Recent genetic discoveries have identified key genes that are active only in ES cells. Working in the laboratory, scientists have used this information to modify differentiated cells to reactivate these genes, in effect regressing the cells into pluripotent stem cells. These cells are known as induced pluripotent stem (iPS) cells, and early research suggests they behave in much the same way as ES cells. Because iPS cells could be created by reprogramming a patient’s own tissues, they lack the ethical concerns posed by ES cells. In addition, because they are a genetic match, therapies using iPS cells would not be rejected by the patient’s immune system. While there are a number of technical hurdles that must be overcome before iPS cells are ready for clinical applications, several companies are beginning to explore treatment possibilities.